Fungal infection of the toenails or onychomycosis is an infectious disease and is a fairly common pathology.The prevalence of toenail lesions in all countries of the world varies from 18 to 45%.Onychomycosis often occurs in elderly people, cancer patients and patients with diabetes mellitus, Kaposi's sarcoma and ichthyosis.
Onychomycosis is not just a cosmetic problem.It poses a serious threat to the human body, since the products (xanthomegnine, viomellein, antibiotic-like substances and penicillin) of the vital activity of the fungus lead to long-term persistence in the affected nails and can lead to the development of hepatopathy, drug-induced toxicoderma and even Lyell's syndrome.
Etiology and epidemiology
The causative agents of onychomycosis are represented by three groups of fungi:
- dermatophytes (up to 95%) - Trichophyton rubrum (causes damage to the nails of the feet and hands, as well as the skin), Trichophytonmentagrophytes (affects the nails on the first and fifth fingers and the skin of the 3-4 interdigital folds), Epidermophytonfloccosum (first and toenails);
- yeast fungi (up to 4%) - Candida spp.(first it affects the skin around the nails, and then it penetrates the nail plate itself);
- mold (up to 1%) - Fusarium and Alternaria (most often found in immunodeficiency states).
Isolated onychomycosis is rare;simultaneous lesions of the skin of the feet, scalp and smooth skin are more often observed.
Infection occurs through household items: bathroom rugs, slippers, towels, manicure accessories;as well as when visiting a spa, sauna or swimming pool.Men are more susceptible to this pathology than women.Mostly adults suffer from onychomycosis;in children, cases of mycosis of the nails are rare.
The risk group includes bathhouse workers, military personnel, athletes, people who regularly visit baths and saunas, and miners.
The source of infection is the skin of the feet of an infected person;sometimes entire families are affected.
Pathogenesis
Onychomycosis is a source of fungal infection that can cause sensitization of the body.In addition, mushrooms release substances that are toxic to the human body.
Predisposing factors for infection are injuries to the skin of the feet and nails that occur when the toes are pinched by tight shoes;humid and warm environment created by some low-quality shoes made of non-natural materials;the presence of serious diseases, immunodeficiency states, old age.
Symptoms of the disease
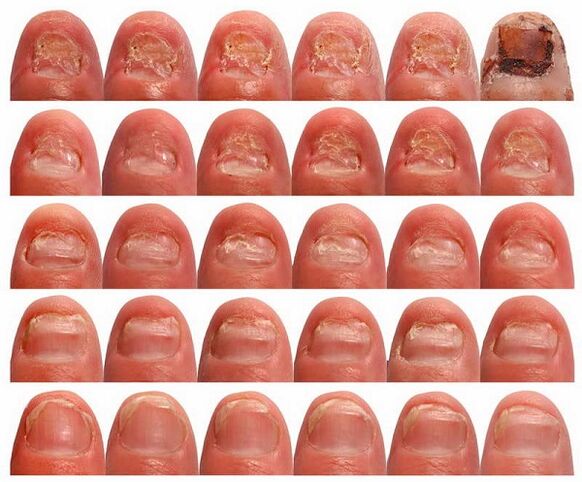
Based on the differences in symptoms, four forms of onychomycosis are distinguished:
- Distal lateral (subungual) onychomycosis.the most common.The causative agents are trichophyton red, candida and, very rarely, mold.With this type of lesion, the fungus in the nail bed enters from the skin through the free edge of the nail and spreads towards the matrix.In this case, the nail plate, due to hyperkeratosis, gradually leaves the bed and acquires a yellow color.Thickening of the nail plate can occur and bacterial contamination gives the nail a variety of colors ranging from green to dirty brown.
- Superficial white onychomycosismost often it is caused by Trichophyton mentagrophytes, which causes the formation of white spots on the surface of the nail plate;as the process progresses, these points merge.This type of onychomycosis occurs in elderly patients with toe deformity, in which one toe covers the adjacent one.The nail plate becomes dystrophic, crumbles and has a gray or brown color, but the matrix and epithelium of the bed are not affected and there are no inflammatory phenomena from the skin either.
- Proximal subungual onychomycosisthe rarest type in which the pathogen, most often red trichophyton, penetrates the nail plate from the skin or from the periungual fold, then spreads along it and reaches the matrix and distal parts of the nail plate.As a result, extensive detachment of the nail plate is observed.With secondary bacterial contamination, the nail plate changes color.
- Total dystrophic onychomycosisdevelops as a complication of distal lateral subungual or, much less often, proximal subungual, and also occurs in chronic subcutaneous candidiasis.With this form, the entire nail is affected with complete destruction;the nail fold is either absent or pathologically thickened, while a normal nail plate cannot be formed.
All onychomycoses must be differentiated from psoriasis, eczema, lichen planus and other skin diseases.To confirm the diagnosis, it is necessary to perform a microscope of the pathological material from the lesion and culture of the pathogen in special identification media.
Treatment of onychomycosis
When prescribing treatment for a patient with onychomycosis, a number of factors must be taken into account: the type of pathogen, the prevalence of the process, the general condition of the patient and his financial capabilities.
- Local agents are often used in the treatment of distal and lateral subungual onychomycosis when no more than 3 nails are affected, as well as in patients for whom tablet types of antifungals are contraindicated.The most effective preparations for soils include creams and varnishes.They are often combined to achieve a faster therapeutic effect.Preparations contain high concentrations of active ingredients;they work effectively on the surface of the nail plate, but are not always able to penetrate the nail bed, where the most persistent fungi are located.In such cases, the affected nail plate is removed either surgically or with the help of special chemicals - keratolytics, and local treatment continues.This method is inconvenient only because of the duration of the process, as it requires careful adherence to the treatment regimen throughout the time during which a healthy nail plate grows.In this case, ointments should be applied every day, and varnishes only once a week.
- Systemic therapy is more effective and reliable in the treatment of onychomycosis;used when local treatment fails.The indications for the prescription of systemic drugs are the late stages of distal and proximal subungual onychomycosis, as well as total onychomycosis.
The choice of drug for systemic treatment should be justified, taking into account the pharmacokinetics, spectrum of action and antifungal activity of each drug.It should not be forgotten that any medicine can give a pronounced therapeutic effect if it is prescribed adequately.
















